The Gut-Brain Axis, Microbiome, Interoception And Reward
- Ana

- 16 hours ago
- 8 min read
Everything seems to be connected.

The gut-brain axis and the emerging absolutely fascinating connections between the gut microbiome and our mental functioning is not something I specialise in. But the research that is coming out at this point is so big, so important and so bloody fascinating that I just cannot resist. I am in absolute awe as to its very actionable therapeutic potential. This will be true even for therapy - through introducing the nutrition-informed aspect to the therapy process. When it comes, it will make therapy only more holistic, attending to the entire person, body-mind-and-soul, as opposed to only its verbal manifestation. But beyond all this, it fascinates me maybe even more for how it reframes our thinking about the mental processes, drilling another big hole into the Cartesian divide.
However, as this fascinating area of enquiry into the architecture of what we are makes important inroads in knowledge, I am fully expecting it becoming a very busy neurobollocks highway - and indeed it probably already is, although as state before I don’t specialise in this area and as a result am less familiar with its own accompanying strain of neurobollocks, the gut-brain-neurobollocks.
This is why it is important for us, as clinicians or even as anyone else really interested in fascinating links between the body and the mind, to keep an extra careful eye on what is what and use sources that are coming from research and not those making cognitive shortcuts in an attempt to provide quick solutions and silver bullets. Like everything else, we are as complex as creatures as our underlying biology is. So, for me, the same rule I apply across all neuroscience stuff I try to fathom, in this field applies too: oversimplified narratives might be seductive and appealing but are unlikely to be true. In other words, there are no silver bullets.
This does not mean that can’t be curious. In fact, we should!
I will try to model this by walking you through some of the compelling ideas I found reading a recent systematic and comprehensive review and an opinion piece on the topic of gut microbiome and eating disorders which situates the conversation et the interface between interoception and reward.
This paper is ultimately about eating disorders and the hopes for better treatment that are starting to emerge. I will use it more as an opportunity the whole idea of the gut microbiome into our conversation here in this publication, and to slowly get the conversation going around the interplay between these important systems, the microbiome and ultimately how its state might affect our mental states and behaviours, illustrating their complex interplay.
First Things First - What is the Microbiome?
I know it might be obvious but let’s just go over the basics here. The microbiome is the whole ecosystem of microscopic organisms living in our gut. And, when we say gut in this context - generally it refers to the gastrointestinal tract - esophagus, stomach and intestines.

The microscopic organisms inhabiting the gut range from bacteria, archea (a group of microorganisms different from bacteria that is thought to be precursor to eucaryotes - organisms with a cell nucleus), fungi, viruses, protozoa (another microorganism that is neither the bacteria not a virus and is an eucaryote).
Because it is an ecosystem its thriving, composition and balance between the different species of microorganisms will inevitably depend on what we eat and our overall lifestyle. Including the medication we ingest - antibiotics being an obvious one.
How we know what we have inside of our gut, microbiome-wise? Well, we really did not have a specific way of knowing before development of genome sequencing and before knowing what the genome sequences of different microorganisms were.
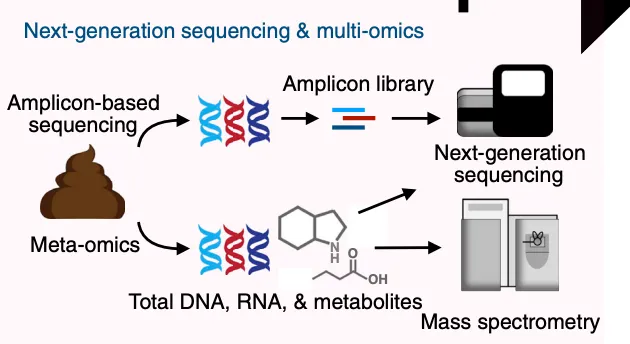
And by yet another technological sleight of hands we can also know about what metabolites these organisms produce - what kind of compounds end up knocking about the gut as a result of their presence. By the same token, if some of these microorganisms are missing or are found in greater or lower concentration - the compounds they synthesise will be missing.
The Complex Interplay
So what is all of the fuss about the microbiome?
The microorganisms might be microscopic but as they are important in the whole cycle of life on earth and the maintenance of ecosystems in the nature the same goes for our internal ecosystem. And this turns out to be true not in terms of physical health only but, importantly for us here, the microbiome has an influence on the brain and its functioning.
So if you remember one thing, remember this - and I quote the original paper here:
the gut microbiome engages in bidirectional communication with the brain through a complex interplay known as the microbiota-gut-brain-axis
Key words being complex interplay. Meaning that probably there won’t be easy solutions to pick and choose from self-optimisation platter. It is more likely yet another layer of complexity to keep in our mind’s and clinician’s eye.
“This communication occurs” - the authors continue - “ through direct and indirect engagement with the vagus nerve, the nervous system, the immune system, neuroendocrine signals, neurotransmitters and microbial metabolites”.
I think this is incredible in and of itself, and there is too much to unpack here, as every of these pathways - the vagal, the immune, neuroendocrine etc - will branch out into its own set of mechanisms of signalling and intersation. To go into any more depth here would either make the whole piece intractable - or create some too dramatic and inaccurate oversimplification. In an effort to avert veering into either of these territories, I will just zoom out and stop here.
From the general health point of view microbiome and it’s abundance and composition, might be important factors in bioavailability - the capacity to absorb the key nutrients such as vitamins and minerals. This process will, of course, have an some effect of mental functioning, if not optimal.
From the general health point of view, when it comes to the gut microbiome, more varied seems to be better. So eat that Kimchi. And all the other weird concoctions.
Interoception and Microbiome
I have written about interoception recently - and so I won’t go into any more detail than just saying that it is the capacity to sense body’s internal states. There is a growing body of formidable work around the connections between interoception, mental states and mental health.
If you would like to know more please refer to my previous piece: Interoception
So is interoception linked to microbiome? If so, do we know how?
Because the satiety/hunger/presence of toxins and other functions linked to the gastrointestinal system are functions that are vital to be signalled to the brain, the gut interoception is a big part of gut-brain communication. As a result, it makes complete sense that microbiome and the presence of all the metabolites of the microbiome will play a role in interoceptive processes.
And microbiome dysregulation can then affect, possibly negatively, the gut-brain related interoception. We can see how that can possibly lead to errors in predictions when it comes to hunger and satiety.
Reward System and Microbiome
First, what is the reward system or the reward circuitry in the brain? Reward is one of neuroscience buzzwords and I think at this point we all know that in some ways it is linked to dopamine.
It is obviously beyond the scope of this essay and of my knowledge, for that matter, to give any form of comprehensive longform lowdown of brain’s reward circuitry. But let me introduce a few ideas, fit for the purpose of this article I think.
Reward is one of those words that have the meaning in the vernacular, in our daily life, that has then been co-opted into the neuroscience which has given it a very specific operational definition - which does not map necessarily completely to what brain actually does (brain does not know what reward is, brain, I think, calculates the value of each and every option and decision we make, base on its estimated survival value or some proxy of it). Also, because dopamine and different addiction narratives have generated so much interest, now operational neuroscience concept of reward has seeped back into the vernacular creating a double confusion. It is a loaded term, for sure.
For our intents and purposes I would say that reward or value are somewhat interchangeable, in this context. It is something that would be deemed positive for survival by the brain and therefore would elicit a positive feeling, generating a positive reinforcing loop. Wolfram Schultz, one of the pioneers of research in neurophysiology of reward and the role of dopamine says the following:
“Rewards make us come back for more. We need them for survival, use them for behavioral choices that maximize them and feel good about them.”
So when we speak about brain reward system - also called the mesolimbic pathway - it refers to the brain circuits that are involved (or ‘activated’) when one is engaged in behaviour that generates the reward. Some key areas are the striatum (nucleus accumbens) and the prefrontal cortex - see the picture below.

Now, back to gut and the microbiome -what is the connection with the reward system?
So, of course, food is so closely linked to survival that it is bound to be rewarding - if we follow the premises from above about what reward is. And indeed this is mediated through the mesolimbic pathway - the reward system - described above.
And the microbiome? Well, in turns out that there is an emerging body of work to support the idea that a ‘messed up’ microbiome can disrupt and mess up the dopamine signalling in the brain that might account not only for some aspects of disordered eating but also for other emotional and motivational presentations. Microbiome, for example, plays an important role in maintaining optimal levels of availability of dopamine (bioavailability) and its depletion, through antibiotics use, can have an impact thus on optimal functioning of dopamine circuits.
Experiences, experiences!
In the beginning of this piece I told you that I don’t know all that much about this topic - although I sure find it fascinating - and so you might know way more than me. If there is anything I or others should have a look at - just make it science supported, pretty please - let me and others know in the comments. You might have your own experience that is linked to this whole story. I would love to hear it!
On a personal level, I know that what I eat hugely affects the state of my body or at least how I feel in my body, the felt sense of it. As a result, my mental states are hugely affected by what I eat and I learned to avoid the bad stuff - the usual suspects - as the repercussions in the aftermath are just not worth the fleeting pleasure. BUT in recent years, I have introduced into my diet a multitude of fermented foods and paid attention to how I feed my pet microbiome (probiotics). I eat kimchi (I make kimchi!), I take kefir and kombucha has become a staple. But, while I love these foods now and relish their subtle textures and pungent aromas, I cannot really say that it has improved, in and of itself, my mental health or that I even noticed any changes in the way I feel - mentally. That, in itself, does not mean much - there is so many confounding variables there, and everyone is different, - but it means that I cannot talk about the link between the augmented microbiome and its effects, from a personal experience.
So I would be eager to hear any experiences of yours - if you care to share.
Before I leave you, I also want to stress the fact that the original piece is really good and so I encourage you to read it.
As always, thank you for reading 🙏.




Comments